Cardiac Catheterization Laboratory (Cath Lab)
Diagnostic and therapeutic procedures for a healthy heart
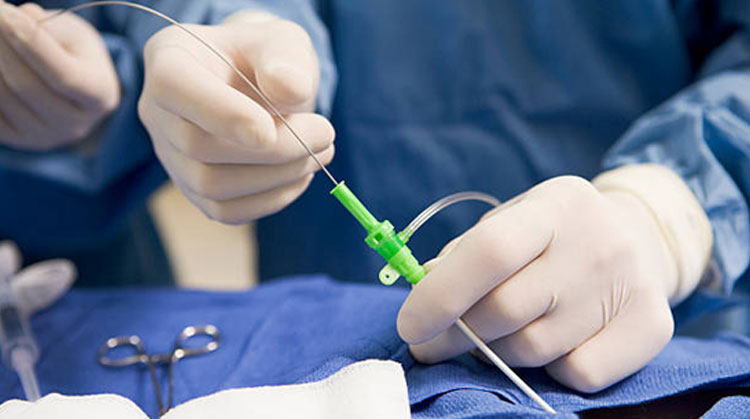
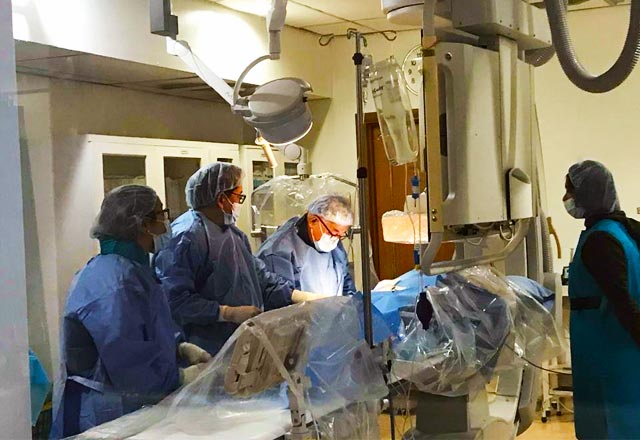
The CMC Cardiac Catheterization Laboratory Complex – or the Cath Lab – is a specialized unit located in the second floor of CMC V. Using X-ray imaging, it undertakes invasive diagnostic and therapeutic procedures on the cardiovascular, cardiac structural, cerebral, renal, and peripheral vascular systems. A specialized group of invasive/interventional cardiologists, radiologists, neurologists, cardiovascular surgeons, and anesthesiologist compose its staff. Trained Cath Lab nurse technologists and radiology technologists contribute to smooth operations in the unit.
Services at a Glance
- Coronary angiography
- Percutaneous coronary interventions, including rotational atherectomy
- Peripheral vascular diagnostic and interventional procedures
- Renal vascular interventions
- Cerebral angiography and interventions
- Peripheral arterial and venous interventions
- Insertion of inferior vena cava filters
- Pericardial procedures
- Valvular and other structural interventions
- Temporary pacemaker insertion
- Permanent pacemaker implantation
- Insertion of various vascular access catheters/devices under ultrasonographic guidance
Conditions that can be detected in a Cath Lab typically include:
- Coronary artery disease
- Congenital heart disease
- Valvular heart disease
- Peripheral artery disease
- Sick sinus rhythm
Lab Facilities
The following are always available at the unit and can be operated instantly on demand:
- State-of-the art imaging system and technical supplies/consumables ensuring safe and highly successful results
- Intra-aortic balloon counterpulsation machine
- Rotablator
- Portable ultrasonography equipment
- Cardioverter-defibrillator
- Pacemaker/pulse generator for temporary pacing
The facility includes an Observation Unit that can hold up to three beds used for pre- and post-operative care of patients. A viewing room with an online real-time monitor is provided for the relatives, family, or companions of patients, where they can view the procedure as it happens and where the operators, through the visual aid, can afterwards discuss with or explain to them the case.
The Cardiac Catheterization Laboratory continues its well-rated service and aims to further enhance the quality of all the various procedures offered, with patient safety, comfort, and affordability as prime considerations.
Specialty Clinics
Ask a question
Quick Contact
- Address Quezon Avenue Cor. Scout Magbanua St., Quezon City, Philippines, 1103
- Email info@capitolmedical.com.ph
- Phone (+632) 8372-38-25
local 4262 - Fax (+632) 411-43-20